Or may be secondarily associated with lung or pleural-based Secondary pnuemothorax may occur iatrogenically with procedures Lung defects are more likely to be caused by other etiologies. Unilateral, matching lung defects are unlikely to represent pulmonaryĮmboli, especially if the other lung is normal or only has Lung, when compared with the same area on the ventilation images.ĬXR: Standard chest radiograph obtained after worrysomeįindings on the ventilation/perfusion scans demonstrateĪ large, secondary pneumothorax, with marked collapse of the Overall, perfusion is slightly better to the right lung Perfusion defects are noted in the left middle and upper lungįields. View demonstrates the anterior-posterior extent of perfusion Of the right lung on anterior and posterior views. Vertical-band of activity extending along the medial aspect In addition, perfusion images demonstrate a The left lung base in a pattern matching the ventilationĪbnormality. Perfusion: Perfusion images demonstrate hypoperfusion to Upon careful inspection, a photon defecient area encompassing much of the expected area of the right lung, with overall less activity than the normal background is seen. Essentially noĪctivity is appreciated in the right lung on washin images.įaint activity can be appreciated along the right hilum To the left lung base on washin images, and significant Ventilation of the left lung, with relative hypoventilation
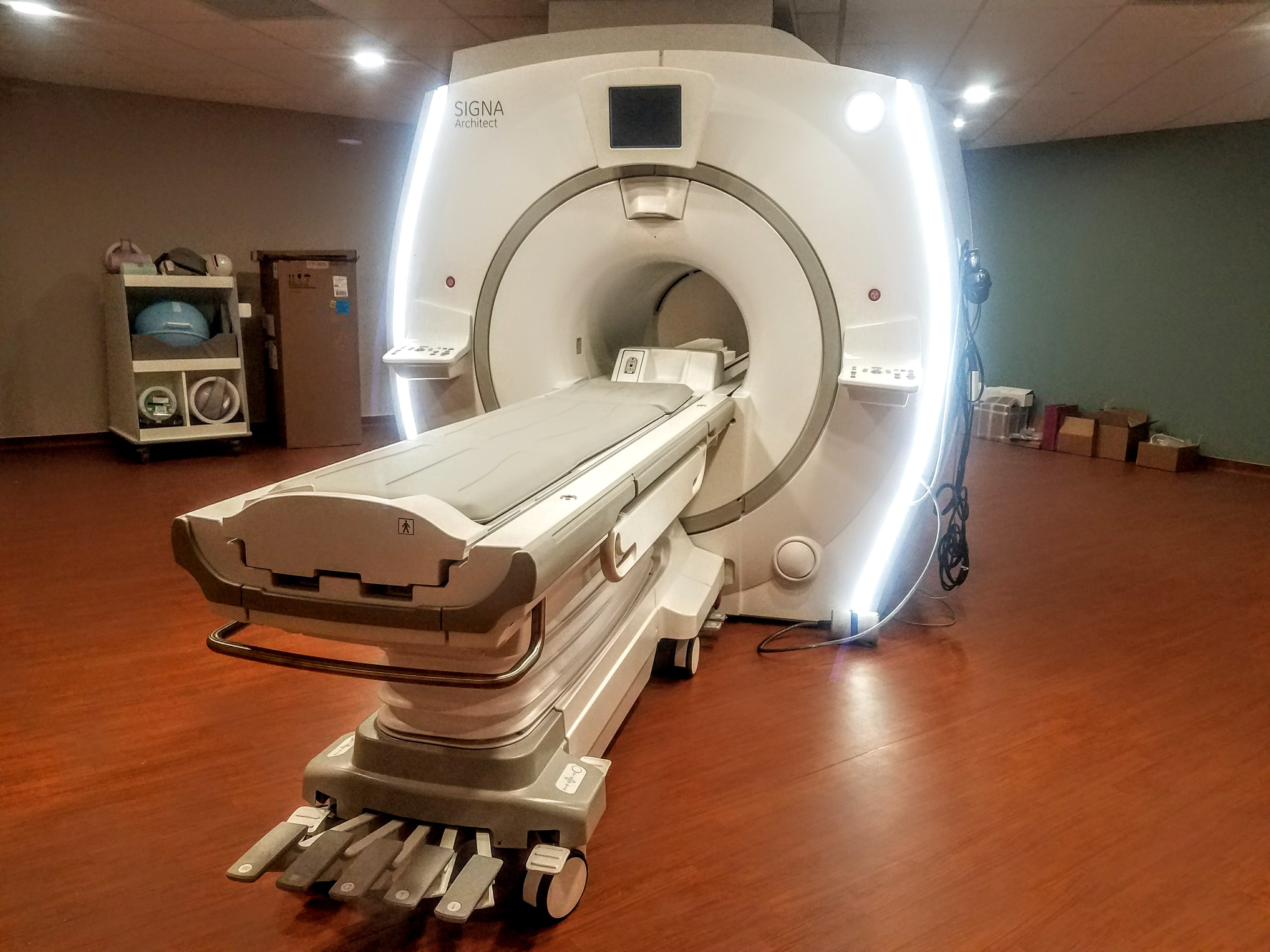
Ventilation: Xenon-133 ventilation images shows abnormal Obtained after the scintigraphic evaluation. Was ordered to rule out pulmonary embolism. With acute worsening of shortness of breath. View main image(vq) in a separate image viewerįull history/Diagnosis is available belowħ1 year old man with a known right hilar mass presented Sheffield The European Respiratory Society.Case Author(s): Vreeland, M.D. , (2015) European Respiratory Society Practical Handbook: NIV.
#DIAGNOSTIC VENTILATION CENON UPDATE#
, (2012) ‘Non-invasive Ventilation in Motor Neurone Disease: an update of current UK practice’ Journal of Neurology, Neurosurgery and Psychiatry 83: 371 -376 Simonds, A. Clinical guideline NICE (2016) Motor Neurone Disease: assessment and management O’Neill, C. August 18 (5 -6): 388 -396 NICE (2010) Motor Neurone Disease: non-invasive ventilation. , et al (2017) Advance Care Planning for patients with ALS fronto-temporal Degen. ‘Existential concerns for people with MND: who is listening to their needs, priorities and preferences? BJOT 79 (6) 391 -393 Levi. BMJ supportive and Palliative Care 4: 43 -39 Harris, D. ‘Issues for Palliative Medicine doctors surrounding the withdrawal of NIV at the request of a patient with MND: a scoping study’. , (2015) ‘Withdrawal of assisted ventilation at the Request of a Patient with Motor Neurone Disease’. Lancet Neurology 5: 140 -7 British Thoracic Society Standards of Care Committee (2002) BTS Guideline: Non-invasive ventilation in acute respiratory failure. , (2006) 'Effects of non-invasive ventilation on survival and quality of life in patients with amyotrophic lateral sclerosis: a randomised controlled trial'. Amyotrophic Lateral Sclerosis and Other Motor Neuron Disorders 3: 145 -149 Bourke, S. , (2002) ‘Non-invasive ventilation in motor neuron disease: current UK practice'. Palliative Medicine 27(6) 516 -52 Bourke, S. (2013) ‘The use of NIV at end of life in patients with MND’. References BBC Inside the Ethics Committee (2011).

